Disclaimer: Throughout the U.S. and spanning the globe, stem cell research and the science of Regenerative Medicine is gaining acceptance and support as an important part of the future of advanced medicine. The good people who work for State and Federal agencies who regulate clinical medicine are trying the keep pace with the rapid advancement of the field. Thus, Federal and State laws and regulations are mercurial, and constantly evolving. Treatments that are allowed today, might be illegal next week. Unfortunately therefore, you might have to leave the U.S. to find the preferred treatment you are seeking. For questions, feel free to call us at: 949-428-4500 or use our online consultation form.
New bio-medical scientific studies have recently discovered that stem cells can be used medically to recreate live healthy tissue to replace damaged or diseased tissue.
In other words, instead of repairing a damaged liver, shoulder joint, or heart, imagine if you could simply create a new liver, shoulder joint or heart!
That is why there is so much popular “Buzz” about stem cells these days. Major universities all over the world are now involved in conducting scientific research on stem cells in order to discover more about these elemental cells and the way they function.

A vial of stem cells being removed from cryogenic storage.
Stem cells can be collected from several sources in the human body, and once they have been properly prepared, Regenerative Medicine specialists around the world report they can provide useful – even miraculous – treatments for all organ systems of the human body. In this comprehensive post, we will discuss more about this complex, compelling, exciting and life-changing topic.
What are Stem Cells?
Stem cells refer to “original” cells that are “undifferentiated” which means they have not yet become cells that are a part of a specific organ system. In fact, stem cells have the potential to become “differentiated” and become specialized cells that are transformed into different organs tissue.
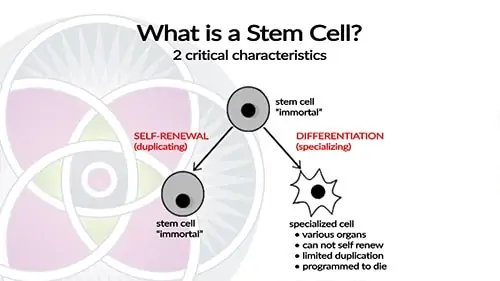
When a stem cell divides, it splits into 1. a copy of itself (self-renewal) and 2. a specialized cell (differentiation).
Like the cells of any organ such as your kidney, skin, or liver, differentiated cells have a specialized purpose that perform a specific function.
Before stem cells differentiate into specialized cells, they can divide through the process of mitosis which leads to the production of more stem cells. This is called the self-renewal capacity which ensures that every organ in your body always has enough stem cells in it that can create, repair and replace tissue that is damaged, diseased and no longer functioning properly.
Humans have two types of stem cells: embryonic stem cells and adult stem cells.
Human Embryonic Stem Cells
Human embryonic stem cells (hESCs) are the initial group of cells that comprise the embryo during the first few days after conception. Each of these embryonic stem cells has the potential to differentiate into every type of human cell and all the organ systems of a developing baby.
hESCs can be expanded in the lab forever (the creation of more cells). As a result, they hold enormous promise for developmental research, drug screening, cell-based therapy, and disease modeling. A thorough understanding of the signaling processes driving hESC differentiation into early cell lineages is critical. Significant progress has been made in understanding the growth factors, intracellular pathways, and transcriptional regulatory networks that regulate hESCs self-renewal and differentiation processes.
Human embryonic stem cells exist only in human embryos that are no more than 1 week old. In other words, embryonic cells can be found only during the very first week of the development of a human’s embryo. This first week of development is called the blastocyst stage.
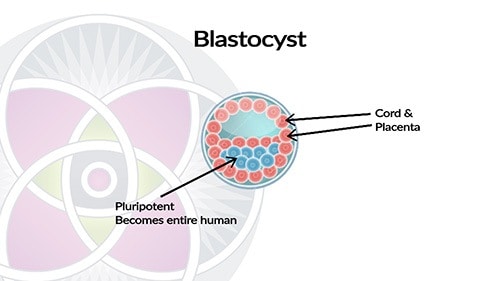
During the first week of embryo development, called the blastocyst stage, is where embryonic stem cells are procured. This stage also contains what will become the placental stem cells or Mesenchymal Stem Cells (MSCs).
In the medical world, these embryos usually come from In-Vitro fertilization clinics, where human eggs are fertilized with human sperm under laboratory conditions and then frozen for future implantation into the mother when she is ready to carry a baby.
After the first week of development, the blastocyst develops two layers of cells: the outer layer of cells forms the placenta, amniotic fluid and the umbilical cord, while the inner layer will eventually differentiate into different cell “lineages” in order to create all the necessary structures and organs of a complete human baby that will grow into an adult (see above image). All this leads to the production of specialized cells that form the different organ systems.
Embryonic Cell “Line” or Cell “Lineages
As original embryonic stem cells develop, three different “lines” of cell types emerge. The three germ layers – mesoderm, endoderm, and ectoderm – create the cellular blueprint for all the tissues and organs that will form during embryonic development. Normal embryonic development requires the precise creation of all three layers as well as the complex signaling between each of them.
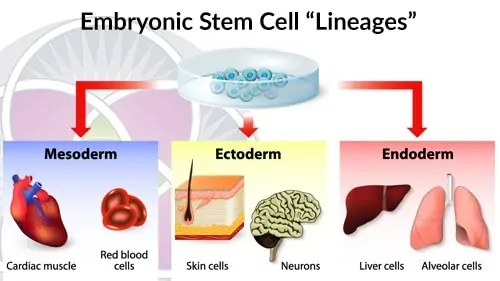
Embryonic stem cells develop into 3 different “lineages”.
Endoderm (inner layer)
During embryonic development, the endoderm is the innermost germ layer that develops the linings of the respiratory and gastrointestinal passages, as well as their related organs such as the liver and pancreas.
Mesoderm (middle layer)
Mesodermal cells are the most prevalent in the human body, representing a wide range of cell types such as the musculoskeletal system (bone, cartilage, and muscle), cardiovascular system (heart, blood, and blood vessels), and connective tissues.
Ectoderm (outer layer)
Organs derived from embryonic ectoderm include mammary glands, CNS, external ear, melanocytes, cornea, brain, nerves, teeth, eyes, and the epithelium of the skin.
Every cell in a human body comes from one of these three fundamental cell lineages.
Human Adult Stem Cells
The second category, Adult Stem Cells, are the stems cells that can be found in each of the developed organ systems. These organ specific stems cells, are in charge of repairing and regenerating new cells and tissue of their specific organ.
For example, stem cells found in the liver take care of liver cells, and can generate new liver tissue whenever needed. Accordingly, kidney stem cells do the same for kidneys, and skin stem cells do that for skin. Thus, each organ system has stem cells that are specifically programed and equipped to care for, repair and regenerate tissue of that organ.
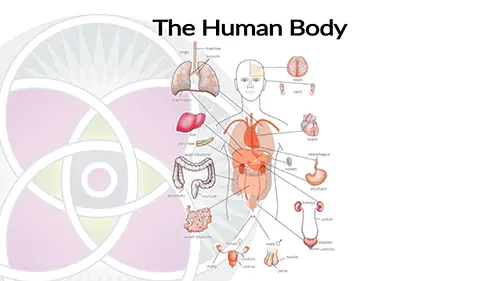
Each organ system has adult stem cells that are specifically programed and equipped to care for that organ.
Adult stem cells that are found in different organs are also known as “somatic” stem cells. They can remain in a non-dividing state for years. However, when the organ tissue becomes injured or diseased the stem cells become activated and start dividing. These somatic/organ stem cells have the capacity to divide indefinitely in a process called “self-renewal”.
Current scientific understanding reveals that adult stem cells, as a group, can only supply derivative cells indefinitely if they are replenished through cell division. Self-renewal is defined as a balanced combination of stem cell division and differentiation that results in a relatively constant number of stem cells. Importantly, both the essential replenishment function of adult stem cells and the associated “self-renewal” traits of differentiation, division, and lifetime persistence apply to the stem cell community within that organ as a whole. They are not always applicable to each individual stem cell.
Whether or not stem cells from a specific organ can also become other types of organ cells and tissues is still a controversial and debatable subject.
Harvesting Adult Stem Cells
When a doctor needs human adult stem cells to treat a patient, where do these stem cells come from? There are three places in the body of the patient where a doctor can collect (“harvest”) the patient’s own adult stem cells:
Bone marrow
These stem cells can be harvested by extraction, which involves drilling into the patient’s bone, usually the iliac crest bone (part of the pelvis bone just above the hip), or a leg bone (Femur, in the thigh – or Tibia, below the knee). As you can imagine, this is not a very pleasant procedure.
Bone marrow transplantation can cure numerous blood illnesses as well as other diseases, such as solid tumors.
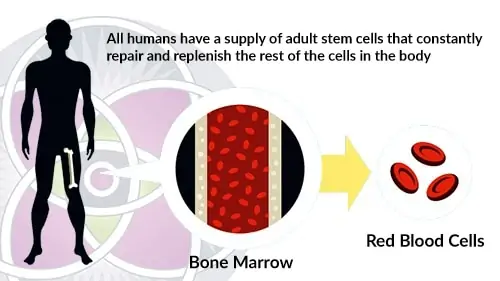
Adult stem cells can be harvested from the patient’s femur bone
Lipid Cells
Because of their abundance in fat tissue and simplicity of extraction via liposuction, adipose-derived mesenchymal stem cells (ASCs) are of great interest. Stem cells found in the adipose (fat) tissue require extraction by liposuction. This too is not a very pleasant procedure.
Furthermore, ASCs can grow rapidly and release significant quantities of pro-regenerative substances. Pilot investigations with human ASCs in vivo have demonstrated their potential to mend calvarial abnormalities and improve vascularization of composite ischemic tissue.
ASCs offer several major advantages over other MSC populations, including the diminishing quantity of BM-MSCs available with age, the vast amounts of bone marrow required, and the procedural hazards associated with bone marrow harvest.
Peripheral Blood
Increasing data suggests that, in addition to BM, peripheral blood (PB) may be a source of stem/progenitor cells for clinical use, including haematopoietic stem cells, endothelial progenitor cells, and MSCs.
Adult stem cells have been found to patrol the bloodstream and circulate across peripheral organs, both healthily and pathologically, which may be essential for tissue homoeostasis and tissue repair. At a steady state, MSCs are present in the peripheral circulation at a relatively low frequency.
However, in response to injury signals, the number of MSCs in the bloodstream increases rapidly. Thus, in recent years, PB, which may be collected with minimum invasion, has been recognized as an important alternative source of MSCs for cell therapy.
Processing Adult Stem Cells
In each of the above 3 processes, the harvested tissue must pass through specialized machines where the harvested stem cells are cleansed, purified and concentrated in preparation for being re-introduced back into the body of the donor, who is also the patient.
Depending on how the prepared stem cells are being administered, they may be prepared in different ways and combined with different formulations.
Important Characteristics of Stem Cells
The two most important characteristics of Stem Cells, and that make stem cells so important to the development of Regenerative Medicine are:
Self-renewal of Stem Cells
This refers to the cells’ ability to go through unlimited cell division cycles while keeping their undifferentiated state. Thus each new generation of stem cells is duplicated by identical new generation of stem cells.
Potency of Stem Cells
Cell potency is stem cells’ ability to differentiate into specialized cell types as part of the tissue of a specific organ.
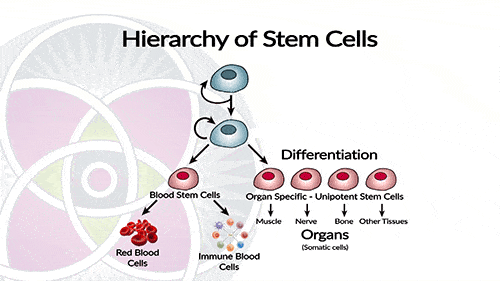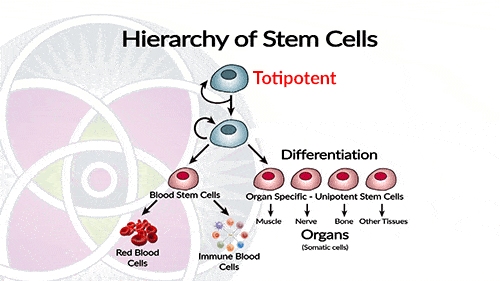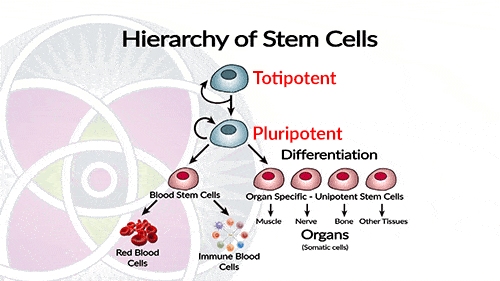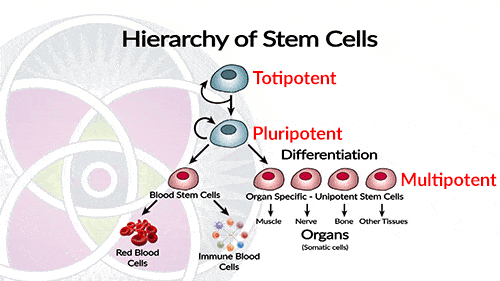
Stem cells can have one of the following potencies, totipotent, pluripotent and multipotent.
Stem cells can have one of the below-presented potencies:
Totipotent Stem Cells
Cells that have the potential to create all cell types including placental cells. Only the earliest of cells of an embryo during the first 4-5 days after fertilization are totipotent.
Pluripotent Stem Cells
These stem cells can transform into all the cell types that will differentiate into specialized tissues that develop into the various organs of a complete human.
Multipotent Stem Cells
These cells will only make certain cell types, being quite limited in their capacity. Generally speaking, the stem cells that exist in an organ, such as a liver, pancreas or skin, are designed to only produce new liver, pancreas or skin cells/tissue.
Sources of Stem Cells (one is not used in medicine)
1. Embryonic, or Fetal, Stem Cells
There are two major problems associated with the use of embryonic, or fetal, stem cells.
Ethical Concerns of Embryonic Stem Cells
As these cells can be obtained only from a developing human fetus, they necessarily involve interfering with the potential development of a human being. This is an ethical mine field and should be.
Biological Concerns of Embryonic Stem Cells
As these cells still retain their pluripotent potency, they can develop into any kind of adult tissue. Therefore, there is a significant risk that if these cells are inserted into an adult, that the wrong kind of tissue might develop.
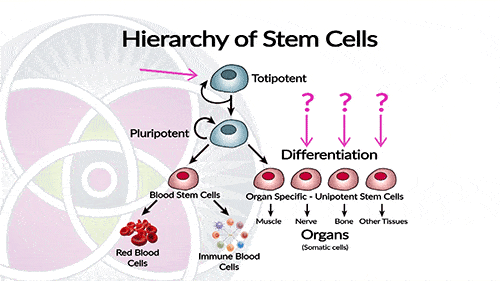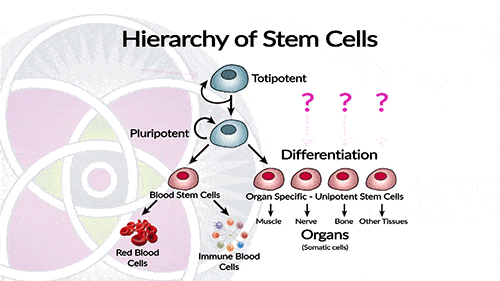
Fetal stem cell are dangerous because they can develop into any kind of adult tissue.
The most serious problem about the clinical use of embryonic stem cells is their tumorigenicity. This may not be surprising considering their innate capacity for fast proliferation and the fact that teratoma formation is the gold standard for measuring pluripotency, but multiple studies mention that they also collect mutations and chromosomal abnormalities in culture.
In certain ways, embryonic stem cells resemble cancer cells rather than regenerative/reparative cells. Their proclivity for proliferation and tumorigenicity is a concerning, if not insurmountable, barrier to their clinical utilization.
Say for example, these cells are injected into a damaged or diseased human liver in hopes that they will generate new liver tissue, but instead, bone tissue is created. Obviously, this unintended consequence could be very detrimental.
Therefore, as a general rule, fetal stem cells are considered dangerous and are NOT used in clinical medicine.
2. Adult Stem Cells
Adult stem cells found in fully formed human organs, whose purpose is the repair and regeneration of that specific organ. Though all adult stem cells share certain characteristics, modern science is discovering that they also differ from each other in distinct and important ways.
Most Commonly Used Adult Stem Cells
The most commonly utilized adult stem cells are extracted from either bone-marrow, fat, or blood. These stem cells have fully developed and unique cellular identity of the person from which they were harvested, and therefore will cause an immunological rejection if introduced into any other human.
Therefore, adult stem cells can only be utilized by the person from whom they were harvested.
3. Placental Tissue or Umbilical Cord Stem Cells
Placental tissue includes the placenta, amniotic fluid and the umbilical cord. This tissue is unique in that it is not part of the developing embryo nor does it belong to the mother.
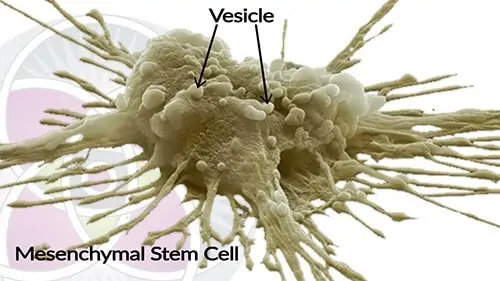
Image of a Wharton’s jelly mesenchymal stem cell harvested from the placental tissue.
Also know as Wharton’s Jelly stem cells, they are not programed to become specialized organs like all other stem cells. These stem cells have essentially already reached their final developmental destiny, and upon the birth of the baby, all the placental tissue is discarded.
And yet, the placenta, the amniotic fluid, and the umbilical cord have stem cells that can be harvested at the same time the baby is born.
Umbilical Cord Stem Cells are Immune Privileged
As these stem cells do NOT genetically belong to the mother, baby, or father, they do not have a genetically distinct identity that would make them incompatible with other humans. Therefore, they CAN be used medically for other adult humans without causing immunological rejection.
These placental stem cells have additional biochemical and cellular characteristics that make them different from other stem cells, and most promising for the advancement of Regenerative Medicine.
What are Stem Cells Used For?
The advancement of Stem Cell research is an increasingly important area of the medical field. Regenerative Medicine specialists around the world report they can replace or heal damaged cells or tissues in the body. You can even say they work as a built-in repair system for the entire human organism.
Human Adult Stem Cells
Adult stem cells have been used in human treatments and stem cell therapies for many years.
Adult stem cells are called the body’s “natural” solution by Regenerative Medicine specialists around the world. This is because they can be found in our bodies in their natural form. When any part of human physiology is in need of healing due to a disease or damage, these cells provide a repair mechanism to replenish your tissues.
Despite research on the potency of a wide range of stem cells for wound healing, adipose-derived stem cells (ASCs) appear to have the fewest limitations for clinical applications. Studies suggest that ASCs can improve wound healing by promoting angiogenesis and/or vascularization, modulating immune response, and inducing epithelialization in the wound.
Wharton’s Jelly Mesenchymal Stem Cells
Wharton’s jelly-Mesenchymal stem cells (WJ-MSCs) currently show the most promise for stem cell therapies. They proliferate rapidly, have a wide spectrum of multipotency, and are hypo-immunogenic.
In comparison to bone marrow MSCs (BM-MSCs) and adipose-derived MSCs (ADMSCs), Wharton’s jelly-Mesenchymal stem cells (WJ-MSCs) grow much more quickly and have a similar immunological profile and multipotency differentiation.
In addition, umbilical cords are regarded as medical waste, their clinical usage in stem cell therapy raises no ethical concerns.
WJ-MSCs have showed significant and promising therapeutic potential. Several approaches have been developed to increase the therapeutic potency of WJ-MSCs in cellular therapy. Treatment of WJ-MSCs with pharmacological substances, cytokines, growth factors, hormones, and vitamins has shown promising results in increasing WJ-MSCs potency.
One thing is for sure, the future of stem cell medicine and its discoveries is going to be exciting.
Learn More About the Science of Stem Cells
References - Read the Science Behind Human Stem Cells...
Everything on our website comes from from reputable publications, books and scientific journals, most of which are available on PubMed and other government websites. These include Meta-Analysis’, Randomized Controlled Trials, Clinical Trials, Systematic Reviews, Books and Documents. We encourage you to read the science, in order to separate fact from fiction, so that you can arrive at a full understanding of what is best for your body. We would be honored to be a part of that educational journey with you.
- Kalderon D. Investigating Adult Stem Cells Through Lineage analyses. Stem Cell Rev Rep. 2022 Jan;18(1):2-22. doi: 10.1007/s12015-021-10282-z. Epub 2021 Oct 22. PMID: 34677818; PMCID: PMC8799514.
- Qin Q, Wang T, Xu Z, Liu S, Zhang H, Du Z, Wang J, Wang Y, Wang Z, Yuan S, Wu J, He W, Wang C, Yan X, Wang Y, Jiang X. Ectoderm-derived frontal bone mesenchymal stem cells promote traumatic brain injury recovery by alleviating neuroinflammation and glutamate excitotoxicity partially via FGF1. Stem Cell Res Ther. 2022 Jul 26;13(1):341. doi: 10.1186/s13287-022-03032-6. PMID: 35883153; PMCID: PMC9327213.
- Kimura JO, Bolaños DM, Ricci L, Srivastava M. Embryonic origins of adult pluripotent stem cells. Cell. 2022 Dec 8;185(25):4756-4769.e13. doi: 10.1016/j.cell.2022.11.008. PMID: 36493754; PMCID: PMC9761687.
- Maqsood M, Kang M, Wu X, Chen J, Teng L, Qiu L. Adult mesenchymal stem cells and their exosomes: Sources, characteristics, and application in regenerative medicine. Life Sci. 2020 Sep 1;256:118002. doi: 10.1016/j.lfs.2020.118002. Epub 2020 Jun 29. PMID: 32585248.
- Varaa N, Azandeh S, Khodabandeh Z, Gharravi AM. Wharton’s Jelly Mesenchymal Stem Cell: Various Protocols for Isolation and Differentiation of Hepatocyte-Like Cells; Narrative Review. Iran J Med Sci. 2019 Nov;44(6):437-448. doi: 10.30476/ijms.2019.44952. PMID: 31875078; PMCID: PMC6885715.
- Hoang DM, Pham PT, Bach TQ, Ngo ATL, Nguyen QT, Phan TTK, Nguyen GH, Le PTT, Hoang VT, Forsyth NR, Heke M, Nguyen LT. Stem cell-based therapy for human diseases. Signal Transduct Target Ther. 2022 Aug 6;7(1):272. doi: 10.1038/s41392-022-01134-4. PMID: 35933430; PMCID: PMC9357075.
- Salemi S, Prange JA, Baumgartner V, Mohr-Haralampieva D, Eberli D. Adult stem cell sources for skeletal and smooth muscle tissue engineering. Stem Cell Res Ther. 2022 Apr 11;13(1):156. doi: 10.1186/s13287-022-02835-x. PMID: 35410452; PMCID: PMC8996587.
- Elshaer SL, Bahram SH, Rajashekar P, Gangaraju R, El-Remessy AB. Modulation of Mesenchymal Stem Cells for Enhanced Therapeutic Utility in Ischemic Vascular Diseases. Int J Mol Sci. 2021 Dec 27;23(1):249. doi: 10.3390/ijms23010249. PMID: 35008675; PMCID: PMC8745455.
- Broughton KM, Sussman MA. Empowering Adult Stem Cells for Myocardial Regeneration V2.0: Success in Small Steps. Circ Res. 2016 Mar 4;118(5):867-80. doi: 10.1161/CIRCRESAHA.115.305227. Erratum in: Circ Res. 2016 Apr 15;118(8):e34. PMID: 26941423; PMCID: PMC4780229.
- Jones R, Lebkowski J, McNiece I. Stem cells. Biol Blood Marrow Transplant. 2010 Jan;16(1 Suppl):S115-8. doi: 10.1016/j.bbmt.2009.10.035. Epub 2009 Nov 5. PMID: 19896546; PMCID: PMC3086546.